The Injectable Hype
The viral life of Ozempic as a vanity drug
—By Emma Kill
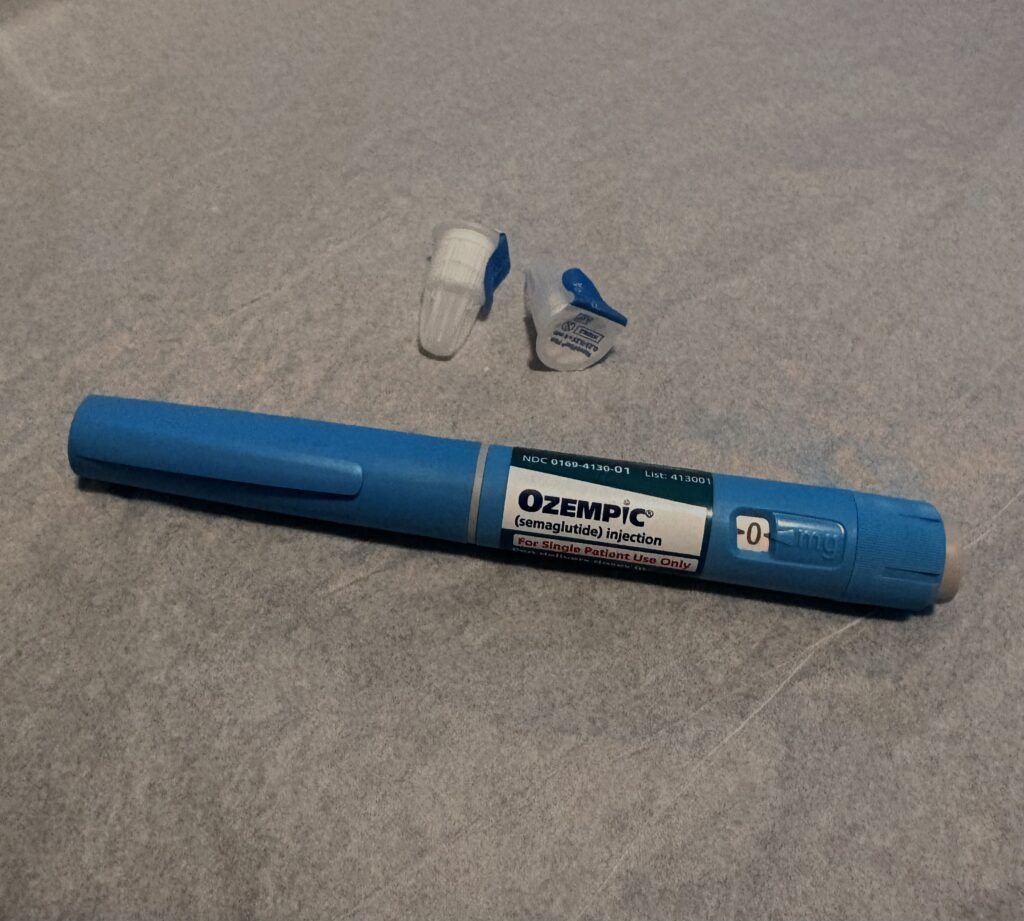
Once a week, patients open their Ozempic kit, remove the syringe cap, attach a sterile needle, and inject the medication into the tissue of their lower abdomen. After holding the needle in place for 3-5 seconds, they dispose of the needle and recap the syringe for next week’s use. My father, Tom Kill, is a type 2 diabetic who is currently on Ozempic. He explains this process as mentally tiresome, always having to remember to “stab yourself” once a week and go through the motions.
This process Kill had described as a chore is now becoming glorified across many platforms. Once a prescription drug designed to manage diabetes, Ozempic has skyrocketed into pop culture fame, thanks to viral TikToks, celebrity endorsements, and countless social media content about its dramatic weight-loss effects. As influencers flaunt their weight-loss transformations, the line between medicine and trend blurs, raising questions about health, accessibility, ethics, and how far people are willing to go for a slimmer silhouette.
How Ozempic works
So what exactly does Ozempic do in the body for those who take it?
Dr. Amy Rothberg, an endocrinologist specializing in diabetes and weight management at Michigan Medicine explains the active ingredient in Ozempic is semaglutide. Semaglutide works primarily within the gut to activate glucagon-like peptide 1 receptors (GLP-1). This reduces gastric emptying and triggers insulin secretion: the hormone associated with uptake of glucose from the blood, lowering blood sugar. Additionally, semaglutide enhances satiety hormones, communicating with the brain that you’ve become fuller faster and suppressing hunger. This also influences the brain’s reward system by diminishing the desire to eat food for emotional reasons and not just physical hunger.
The role of social media platforms
Content shared across social media platforms suggest that Ozempic is mainly viewed as a positive to weight loss. The most controversial part about this view is that Ozempic isn’t an FDA approved drug for weight loss. Its only intent is to manage type 2 diabetes.
A cross-sectional study, “Descriptive analysis of TikTok videos posted under the hashtag #Ozempic” examined the first 100 videos that came up when “#Ozempic” was typed into the search bar of TikTok. The results found the videos were heavily concentrated on personal use and weight loss, rather than providing balanced or medically accurate information. Only a small percentage mention the potential side effects related to Ozempic or other important issues such as off-label use and drug shortages. This promotes the trend-like fashion of the drug which downplays medical-based knowledge and the potential risks.
UM student Lydia King attests to this by saying the type of Ozempic-related content she comes across are mostly “Facebook moms” speaking highly of the drug or videos like “what I eat in a day on Ozempic.” King also notes hearing jokes about Ozempic around campus, suggesting that most young adults are exposed to it in a humorous way. She believes that with growing popularity, “social media videos are not instilling positive practices such as maintaining a healthy lifestyle.”
It’s no surprise that the rise of health-related trends are coupled with the spread of misinformation. Many, if not most people, have assumptions that Ozempic is for weight loss because of marketing advertisements emphasizing that effect. While a loss of weight is a side effect of these drugs, its purpose is to mitigate type 2 diabetes, which we now know. Dr. Rothberg and UM alumni Melissa Drallos, PA in family medicine, both reemphasized that Ozempic is not FDA-approved for weight loss usage. Its medications like Wegovy and Zepbound that have been FDA-approved for weight loss.
Many patients are now asking to be put onto Ozempic and similar drugs because of what they see on TikTok and from celebrities. “If it’s not every day, it’s every week my patients ask about Ozempic,” Drallos recounts. She explains that many patients report the wonders it does for their friends or people on social media, which encourages them to want to be on it too. Drallos will have to tell them Ozempic is not an option for those without diabetes and discuss what alternatives are available instead.
Unfortunately, with the influx of social media popularity, physicians often report that they feel pressured to prescribe medications that patients request and note what little understanding most people have related to these medications. Physicians believe that such advertising leads patients to overestimate a medication’s effectiveness and misinterpret their own medical autonomy. This can disrupt physician-patient relationships by creating conflict when prescriptions are denied.
What does this mean for diabetic patients?
This trend has sparked frustration among providers because their diabetic patients are having difficulties accessing their GLP-1 medications. Drallos had patients calling her almost everyday in 2024 saying their pharmacy was out of Ozempic and would ask if she could send their prescriptions to another pharmacy. Some patients had to call five to six pharmacies or travel to the state over just to find their medication. Many had to be switched to other medications to manage their diabetes. This frustrated Drallos because of the associated risks when switching patients from their current treatment. Kill also reported this issue, testifying to having difficulties accessing his medication and experiencing delays and shortages at his pharmacy.
These shortages are driven by business interests, including startups and medspas promoting semaglutide for weight loss at discounted prices. People also obtain Ozempic from providers prescribing them off label—not for the drug’s FDA approved usage. Dr. Rothberg expresses her concern when people turn to these outlets to access weight loss drugs; “I think we’re [providers and patients] in big trouble.” The elimination of direct medical oversight elevates the inherent risks associated with these services. Treating obesity isn’t a one-size-fits-all solution; many factors play into it.
Pharmacy technician Jungwon Kim said that Ozempic was always out of stock at the pharmacy she worked at. She had to constantly refer patients to other pharmacies, and even they didn’t have it in stock, leaving patients upset. Some people even came to ask to buy Ozempic without a prescription. With that being said, as long as someone had a valid prescription signed by a healthcare professional, she had to dispense it. Due to HIPAA, Kim did not have access to diagnoses for medications, like Ozempic, so there were no protocols in measure to allow priority to diabetic patients during shortages.
In January of 2025, Drallos reported that her medical practice received notices from health insurance companies, like Blue Cross Blue Shield, saying they were no longer covering GLP-1 medications for weight loss purposes because of the increasing demand. This created even more discrepancies for patients who need these medications for combating obesity. Dr. Rothberg explains how there are clear health equity concerns, since many of the people who could benefit most from these medications aren’t able to access them. A large portion of the population goes without treatment simply because they’re uninsured or underinsured. Even if their insurance covers the medication, copays can still be very expensive.
Benefits for combating obesity
Dr. Rothberg believes one positive outcome of media attention to these medication availability is that more people are starting to recognize obesity as a legitimate disease and are seeking treatment for it. These drugs can serve as valuable tools to help patients lose weight and improve their health. Importantly, they may also encourage people who previously avoided healthcare due to stigma to finally seek medical support. Furthermore, Dr. Rothberg testifies that for many, these medications can be highly effective, helping them lose weight and improve overall health. Patients often experience less joint pain, greater mobility, and an improved quality of life.
However, Dr. Rothberg does caution that with every drug comes side effects; GLP-1 medications are no exception to that. Side effects include, but not limited to: nausea, vomiting, constipation, diarrhea, abdominal pain, gastroparesis, and pancreatitis. For many, these effects are intolerable which is discouraging and may affect the trajectory of weight management of obesity for those on Zepbound or Wegovy.
Ozempic isn’t the full solution
Ultimately, while medications like semaglutide—in the context of weight loss—can be powerful mechanisms for improving health, experts emphasize they are not one-size-fits-all solutions. As Dr. Rothberg notes, healthcare providers “shouldn’t be cavalier about prescribing these drugs.” Careful and individualized evaluation is essential to ensure these medications are used appropriately and safely.
There also needs to be a push to supplement these drugs with a change in mindset Drallos urges. It’s not about chasing a number on a scale, but working towards improving overall health; it isn’t a “magic shot” on its own. Yet, in an age where social media glorifies quick fixes, voices like King’s remind us that true well-being comes from balance and considerable effort; “understanding a healthy diet and living healthy is becoming a lost art form.”
Feature photo: Ozempic Vial; Photo Credit, Emma Kill